Shoulder Impingement Syndrome: Overcoming the Pinch for Lasting Relief
Behind the Pinch: Anatomy and Mechanics of a Crowded Shoulder
Shoulder impingement syndrome is one of the most common—and most misunderstood—sources of shoulder pain in adults. The shoulder relies on complex coordination between bones, muscles, tendons, and fluid-filled sacs called bursae to allow effortless movement. At the heart of impingement is a vital structure: the subacromial space. This narrow passage, sandwiched between the acromion (the high point of the shoulder blade) above and the head of the humerus below, houses the critically important rotator cuff tendons and the subacromial bursa.
In a healthy shoulder, these soft tissues slide freely as you lift, rotate, or reach with your arm. However, when this space becomes crowded by swollen tendons, inflamed bursa, bone spurs, or shape changes in the acromion, tissues get pinched, resulting in sharp pain, inflammation, and loss of function.
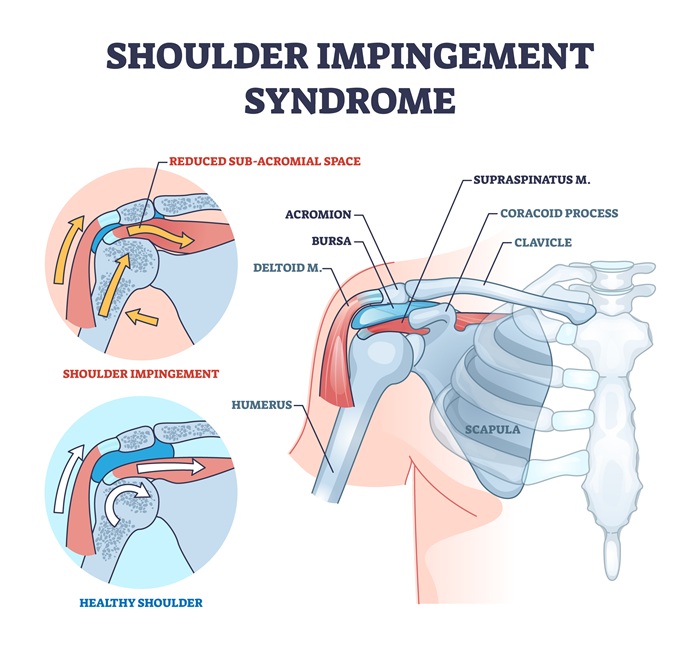
What Actually Gets "Impinged"? Exploring the Subacromial Space
- Rotator cuff tendons: Especially the supraspinatus, which passes beneath the acromion when lifting the arm.
- Subacromial bursa: This lubricating sac cushions the rotator cuff from the bones above.
- Biceps tendon: Less commonly, this structure can also become entrapped.
Anatomic variations, such as a hooked or downward-tilting acromion or the formation of bone spurs with age and arthritis, further crowd this pathway. In some individuals, genetics play a significant role, predisposing people to impingement even without major injury.
Mapping the Causes: How Shoulder Impingement Develops
Shoulder impingement usually arises from a combination of factors:
1. Repetitive Overhead Activity
- Sports (swimming, tennis, baseball)
- Occupational demands (painting, construction, warehousing)
- Household tasks (frequent lifting, window cleaning)
2. Poor Posture and Scapular Control
- Slouching or forward-rounded shoulders decrease subacromial space
- Weak rotator cuff and shoulder blade muscles allow the humeral head to ride high, increasing compression on soft tissues
3. Pre-existing Conditions
- Rotator cuff tendinitis or tears
- Chronic bursitis
- Shoulder instability or previous injuries
4. Degenerative Changes and Age
- Bone spurs (osteophytes) along the acromion or AC joint
- Loss of elasticity in tendons and ligaments
- Arthritis in the acromioclavicular joint
5. Anatomical Variation
- Acromion shape (hooked, curved, or flat): Some shapes create more natural “pinch”
- Thick ligaments narrowing the passage
In younger athletes, impingement often involves internal factors—tight posterior capsule or specific tendon and labrum injuries from repetitive throwing. In those over 40, it more often involves degenerative narrowing, tendon thickening, or bony overgrowth.
Spotting the Signs: Classic Symptoms of Shoulder Impingement
Impingement produces a distinct pattern of discomfort and disability. Common symptoms include:
- Sharp pain or aching with overhead motion, especially reaching, lifting, or throwing.
- Pain is most often felt on the outside or front of the shoulder, sometimes radiating down to the elbow.
- Tenderness to the touch at the front, side, or top of the shoulder
- Night pain, worse when lying on the affected side
- Weakness—especially with lifting the arm out to the side or pushing against resistance
- Stiffness and limited range of motion, causing difficulty dressing, washing hair, or reaching overhead
- Catching, clicking, or grinding sensations with movement
- Achy pain at rest or after activity
Symptoms often start mildly and worsen with continued use or unaddressed biomechanical issues. If untreated, chronic impingement may lead to rotator cuff tears, persistent bursitis, or even frozen shoulder (adhesive capsulitis).
Meet Our Specialists

The Diagnostic Journey: How Shoulder Impingement Is Uncovered
Diagnosis relies on careful medical history, targeted physical exam, and occasionally imaging:
- History: Key questions include onset, activities involved, aggravating and relieving factors, functional impact, prior injuries, and general health.
- Physical Exam:
- Palpation locates tender points.
- Strength and range of motion tests identify weakness and loss of function.
- Special “impingement tests”:
- Neer test and Hawkins-Kennedy test reproduce pain as the rotator cuff is compressed beneath the acromion.
- Painful arc: Discomfort felt between 70–120 degrees of arm elevation.
- Evaluation for rotator cuff tears, instability, or arthritis.
Imaging
- X-rays: Visualize bony changes (spurs, acromion shape, arthritis) but not soft tissue directly.
- Ultrasound: Helpful for detecting thickened tendons, bursitis, and dynamic movement issues.
- MRI: Reveals tendon/bursal inflammation, tears, and helps rule out associated conditions if conservative care fails.
Diagnosis is mainly clinical, but imaging provides essential clarification and is especially important for chronic or severe cases.
The Holistiq Approach: Rehabilitation, Restoration, and Relief
Most cases of impingement can be managed—often fully resolved—without surgery, if caught and treated early. At Holistiq Health, the focus is on restoring healthy movement, reducing pain, and addressing ALL contributing factors through integrated, patient-specific care. We accept all major health insurance, making expert rehabilitation accessible for everyone.
1. Anti-Inflammatory Nutrition
- NSAIDs (ibuprofen/naproxen) and acetaminophen reduce discomfort in the “freezing” stage.
- Ice and heat: Decrease inflammation and promote blood flow as needed.
- Corticosteroid injections: Strong evidence for short-term pain reduction and modest improvement in range. Ultrasound-guided injections boost targeting safety.
- Hydrodilatation: Injection of saline (sometimes with steroid) to stretch the capsule in select cases, shown to accelerate early pain relief and flexibility.
2. Physical Therapy: Restoring Balance and Space
- Custom diet plans to decrease inflammation and support tendon repair
- Focus on omega-3 rich foods, leafy greens, berries, lean proteins, nuts, and seeds
- Minimize processed food and added sugars, which exacerbate inflammation
3. Chiropractic Care and Manual Therapies
Cornerstone of impingement treatment—custom progressive plans include:
- Postural retraining: Teaching the body to maintain neutral, “shoulders-back” position
- Rotator cuff and scapular strengthening: Rebuilding stabilizers to prevent excessive upward movement of the humeral head
- Range of motion drills: Gentle stretching, wall climbs, stick exercises
- Neuromuscular re-education: Ensures proper firing and rhythm of all supporting muscles
- Manual therapy: For mobility improvements and soft-tissue restrictions
- Consistent therapy reverses impingement by creating more space, cushioning irritated tissues, and restoring function.
4. Shockwave Therapy and Modalities
- High-energy sound waves promote healing in persistent tendinitis or bursitis
- Used in chronic or treatment-resistant impingement syndromes
5. Pain Injections
- Corticosteroid injections (guided by ultrasound for safety/accuracy): Break cycles of severe pain and swelling, creating a window of opportunity for therapy
- Limited to a few per year to avoid tendon weakening, always as part of a larger rehab plan
6. Regenerative Medicine
For cases where traditional care hasn’t sufficed, Holistiq offers:
- Platelet-Rich Plasma (PRP): Concentrated growth factors from your own blood, injected at injury site to stimulate repair
- Stem cell therapies (when indicated)
- All non-surgical options are tailored and supervised by experts for optimal results.

Setting Yourself Up for Success: Prevention and Lifestyle Strategies
- Warm up thoroughly before exercise or physical work
- Practice proper lifting, throwing, and reaching techniques—never “shrug” the shoulder during these actions
- Avoid repetitive overhead activities when possible; alternate tasks to minimize overuse
- Strengthen and stretch the rotator cuff and scapular muscles routinely
- Maintain good posture, both standing and sitting
- Take work/task breaks, especially with prolonged overhead tasks
Early intervention trumps toughing it out—persistent “minor” pain often signals brewing impingement.
Frequently Asked Questions About Shoulder Impingement
How is shoulder impingement different from a rotator cuff tear?
Impingement is compression and irritation of the rotator cuff and/or bursa between the acromion and humerus. While untreated impingement can evolve into a rotator cuff tear, the two are not the same—with tears, the tendon fibers are actually disrupted.
Do I need surgery to fix impingement syndrome?
Over 90% of shoulder impingement cases respond to non-surgical management. Surgery, typically a minimally invasive procedure to clear out bone spurs or inflamed tissue, is reserved for those not improving after robust therapy and injections.
Can shoulder impingement come back?
It can—especially if risk factors like poor posture, weak rotator cuffs, or repetitive overhead activities go unaddressed. Prevention and ongoing exercise are vital.
Does impingement require absolute rest?
No. Rest from aggravating overhead activities is essential, but maintaining gentle range of motion and strengthening certain muscles is critical to prevent stiffness and loss of function
Is shoulder impingement covered by insurance at Holistiq Health?
Yes. At Holistiq, all major health insurance is accepted for evaluation, therapy, and most advanced modalities. Regenerative medicine options can also be discussed.
How soon should I seek help?
Persistent shoulder pain lasting more than a few weeks—especially with night pain, weakness, or functional loss—warrants evaluation. Early intervention accelerates recovery and limits complications.
Take Control of Your Shoulder Pain
You shouldn’t have to live with chronic shoulder pain, interrupted sleep, or activity restrictions. At Holistiq Health, you’ll work with leading providers using the most advanced, evidence-based non-surgical solutions. From anti-inflammatory nutrition and top-tier physical therapy to targeted injections and regenerative medicine, our integrated approach personalizes every recovery. We accept all major health insurance and collaborate closely on workers’ compensation and prevention strategies.
Where Does It Hurt? We Can Help.