MSK Costs Are Quietly Taxing Your Operations: How Employers Can Reclaim Cost and Productivity
Musculoskeletal (MSK) issues are treated like “just another medical claim” in many employer reports. In reality, they are one of the most powerful forces shaping your healthcare spend, lost workdays, and day‑to‑day operational stability.
If you run a high‑MSK‑risk workforce—manufacturing, logistics, transportation, construction, healthcare—you’re not just paying for MRIs and surgeries. You’re paying for overtime, missed shifts, slowed production, and a constant scramble to cover physically demanding roles.
This article breaks down where MSK really hits your business and how a structured MSK model like OneMSK can turn a major cost driver into a managed, measurable system.
Where MSK Really Shows Up on Your P&L

Most employers see MSK in one obvious place: medical and pharmacy claims. But the true impact runs across multiple buckets:
- Direct medical costs: imaging, specialist visits, injections, procedures, and surgeries.
- Indirect productivity costs: lost workdays, light‑duty restrictions, overtime to cover absent workers.
- Disability and workers’ comp: longer durations, repeat injuries, and avoidable escalations.
- Turnover and retraining: employees who never fully recover, churn out, and must be replaced.
When MSK care is fragmented—different providers, inconsistent protocols, long waits for appropriate care—minor issues are more likely to become major claims. A sore back becomes a months‑long absence. A shoulder strain turns into surgery that might have been avoided with earlier, conservative intervention.
From the CFO and Finance side, this shows up as an inflated, volatile category that’s hard to predict or control. From the HR, Safety, and Operations side, it looks like chronic staffing friction: open shifts, fatigue, and unstable throughput.
Why Traditional MSK Care Fails Employers
The problem isn’t just that MSK conditions are common. It’s that the way employees access MSK care is misaligned with how high‑risk workforces actually operate. Typical patterns include:
- Delayed access to the right care: Employees start with urgent care or primary care, bounce to imaging, then wait weeks for physical therapy or specialist appointments.
- Over‑reliance on high‑cost interventions: Without a clear conservative pathway, it’s easy to end up with unnecessary MRIs, injections, or surgeries.
- No unified navigation: No one is accountable for guiding the employee from first complaint through rehab and return‑to‑work.
- Site‑to‑site variability: Different locations use different local providers, creating inconsistent outcomes, costs, and experiences.
For employers, that means:
- Higher total MSK spend than necessary.
- Longer disability and workers’ comp durations.
- Higher risk of re‑injury and repeated claims.
- Friction with employees who feel “on their own” in the system.
In short, MSK care is often reactive, fragmented, and driven by where the employee happens to go—not by an employer‑designed model of access, quality, and cost control.
Connecting Cost Control to Access and Experience
A key insight for enterprise employers: you can’t control MSK cost if you don’t control how and where employees access care.
When the only options are ERs, offsite clinics, or long waits for appointments, you get:
- More lost work time just to get basic evaluation and follow‑up.
- More unnecessary imaging and specialist referrals.
- More frustration for employees balancing work, family, and complex care journeys.
By contrast, when MSK care is embedded into the workday and extended virtually to remote or traveling staff, you shift the curve:
- Issues are triaged earlier, before they escalate into high‑cost events.
- Employees can access care without burning PTO or entire shifts.
- Navigation is clearer, with defined pathways and expectations.
Better access and better experience are not “nice to have” features. They are core levers for both cost and productivity.
What an Employer‑Designed MSK Infrastructure Looks Like
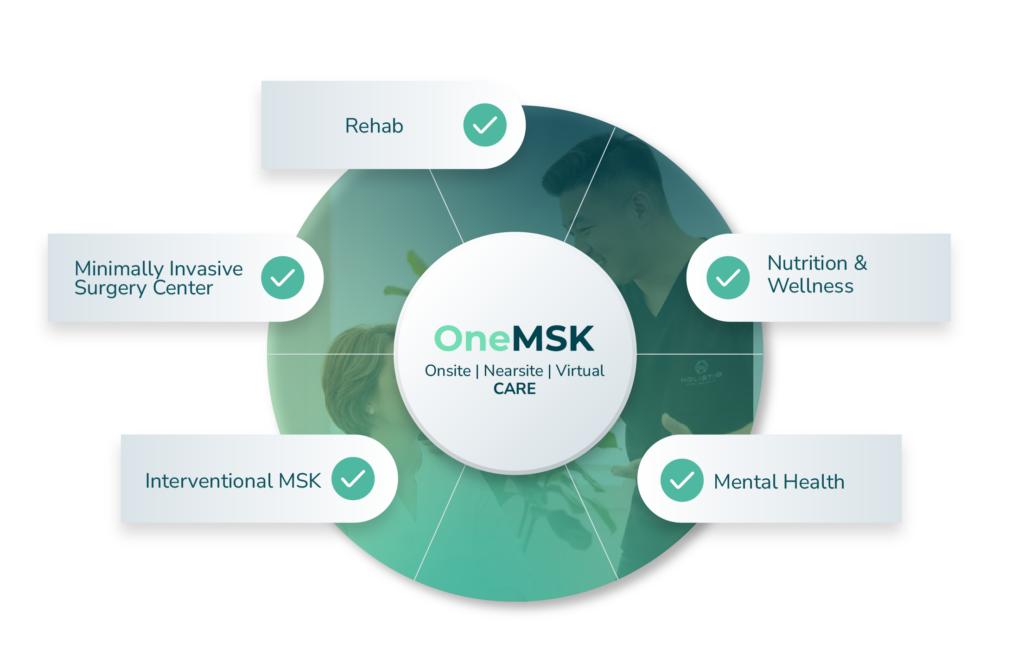
OneMSK is built around the idea that MSK for employers should function as an infrastructure—not a loose collection of point solutions.
A complete employer MSK model includes:
Onsite or nearsite MSK clinics
- Embedded at or near your workplace for triage, assessment, rehab, and care navigation.
- Reduces travel time, ER use, and unnecessary offsite visits.
Interventional MSK and minimally invasive surgery
- Coordinated access to injections, nerve blocks, and minimally invasive procedures when appropriate.
- Standardized pathways and second‑opinion style thinking to avoid unnecessary major surgeries.
Whole‑person support
- Behavioral health for pain, anxiety, depression, and sleep challenges that often accompany chronic MSK issues.
- Nutrition and wellness support, including anti‑inflammatory approaches and weight management.
Analytics and reporting
- Clear visibility into utilization, cost trends, functional outcomes, and employee experience.
- Employer‑ready reporting for HR, Finance, Safety, and broker partners.
Instead of employees bouncing through a maze of uncoordinated providers, they move through a defined, employer‑aligned MSK pathway—from first complaint to full recovery.
When MSK care becomes a structured infrastructure instead of a fragmented cost center, employers can expect:
- Lower total MSK spend
- Earlier intervention and conservative care prevent escalation.
- Standardized pathways curb unnecessary imaging and surgeries.
- Fewer lost workdays and faster return‑to‑work
- Onsite/nearsite access reduces time away for appointments.
- Streamlined surgical and rehab pathways shorten disability durations.
- More stable workforce coverage
- Fewer surprise absences tied to unmanaged pain or long waits for care.
- Better fit‑for‑duty decisions and safer return‑to‑work planning.
- Higher employee satisfaction with MSK benefits
- Convenient access and longer, more comprehensive visits.
- A sense that the employer is actively supporting physical and mental well‑being.
For enterprise leaders, this shifts MSK from “uncontrollable noise in the claims file” to a managed operational lever that can be measured, benchmarked, and improved over time.
How Employers Typically Start

Most employers don’t overhaul everything at once. Common starting points include:
- Piloting onsite or nearsite MSK triage at one or two high‑risk locations.
- Introducing standardized MSK pathways for a specific condition (for example, low back pain or shoulder injuries).
- Aligning with a partner that can integrate onsite, interventional, and surgical components under one coordinated model.
From there, organizations expand to more sites, broaden condition coverage, and deepen analytics so they can demonstrate impact to CFOs, CHROs, COOs, and broker partners.
Ready to Rethink MSK Cost and Productivity?
If MSK issues are showing up in your claims, overtime, and staffing challenges, the problem isn’t just the conditions themselves—it’s the structure of how employees access care.
A unified onsite/nearsite, MSK model gives you a way to:
- Control total MSK spend more deliberately.
- Protect productivity and workforce stability.
- Offer a better, easier experience for employees who rely on their bodies to do their jobs.
To see how an employer‑designed MSK infrastructure could look for your locations, shifts, and risk profile, visit the OneMSK page or request a OneMSK Strategy Call.



