What Does Sciatica Feel Like?
Sciatica often feels like sharp, shooting, or burning pain that starts in your lower back or buttock and travels down one leg, sometimes all the way to your foot. For some people it is a mild ache; for others it is intense nerve pain that makes standing, walking, or sleeping difficult.
How Common is Sciatica?
Sciatica is one of the most common types of nerve-related leg pain. Estimates suggest that up to 40% of people will experience sciatica at some point in their life. Each year, roughly 1% to 5% of adults develop sciatica symptoms, often related to a lumbar disc problem.
Sciatica becomes more frequent in middle age, especially between ages 30 and 50, when disc herniation and age‑related spine changes are more likely. Risk is higher in people who do heavy lifting, sit for long periods, smoke, or have obesity.
What sciatica actually feels like
Sciatica describes symptoms from irritation or compression of the sciatic nerve, usually in the lower spine. Classic sciatica pain starts in the low back or buttock and radiates down the back of one leg, sometimes into the calf, foot, or toes.
People commonly describe sciatica as:
- A deep ache, burning, or throbbing pain in the buttock, thigh, or calf.
- Sharp, stabbing, or “electric shock” pain that shoots down the leg with movement, coughing, or sneezing.
- Numbness, tingling (“pins and needles”), or a sense that the leg or foot is “asleep” along the same path as the pain.
- Sciatica usually affects one side of the body, not both, and symptoms can flare with sitting, bending, lifting, twisting, or driving. In more severe cases, the leg may feel weak or unsteady because the nerve signals that control muscles are affected.

Sciatica Pain So Bad You Can’t Walk
During a severe flare, sciatica can be so intense that standing upright or walking more than a few steps feels impossible. This may be due to severe nerve pain, muscle spasm, or weakness in the affected leg.
- Serious red‑flag symptoms that require urgent or emergency care include:
Sudden or rapidly worsening weakness in one or both legs. - Trouble lifting the front of the foot (foot drop) or dragging the foot when walking.
- Loss of bowel or bladder control or inability to urinate.
- Numbness in the groin or “saddle” area.
These signs can indicate cauda equina syndrome, a rare but serious condition that occurs in about 1% to 2% of herniated disc cases and needs immediate treatment to prevent permanent damage. For very painful but non‑emergency episodes, short‑term strategies like relative rest, ice or heat, and over‑the‑counter anti‑inflammatory medication (if safe for you) can help until you see a clinician.
How to Sleep with Sciatica
Sciatica often feels worse at night because lying in one position for hours can increase stiffness and nerve irritation. Poor sleep can then amplify pain sensitivity, creating a cycle of discomfort and fatigue.
Positioning tips many clinicians recommend include:
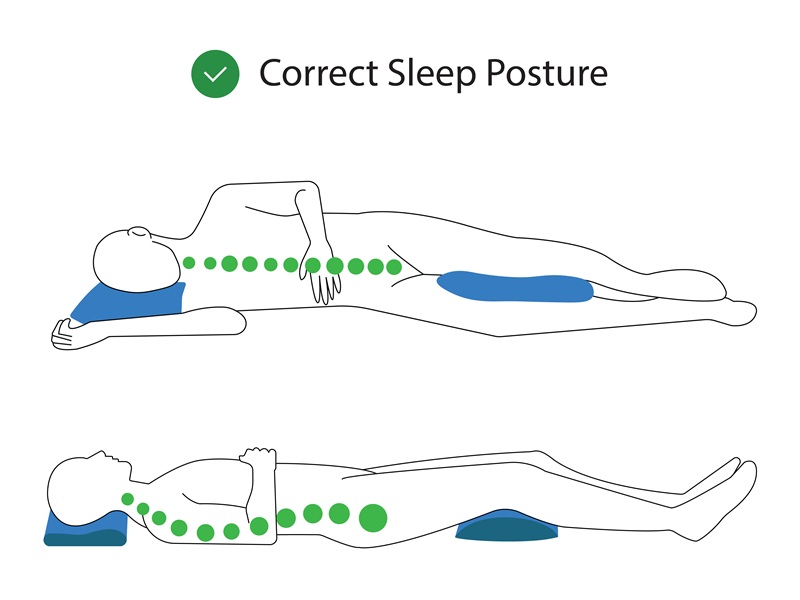
- On your back: Place a pillow under your knees to reduce stress on the lower spine and nerve roots.
- On your side: Lie on the side opposite the painful leg with a pillow between your knees to keep hips and spine aligned.
- Surface: A medium‑firm mattress often supports the spine better than a very soft one that lets your hips sink.
Before bed, a short walk, gentle stretches, or a warm shower can relax tight muscles and reduce night‑time symptoms. Many people also find a 15–20 minute session of heat or cold helpful before lying down, depending on what feels best for their body. Because individual conditions differ, a tailored plan from your clinician or physical therapist is ideal.
Does Sciatica Go Away?
The outlook for sciatica is often good. Studies show that many people with disc‑related sciatica improve substantially within about 6 to 12 weeks of non‑surgical treatment. In some cohorts, more than 70% of patients report significant pain reduction within a few months.
Sciatica is a symptom, not a disease, so how long it lasts depends on the underlying cause—such as disc herniation, spinal stenosis, bone spurs, or degenerative disc disease. Common components of conservative care include:
- Staying as active as possible, with short rest periods rather than prolonged bed rest.
- Medications such as anti‑inflammatories, nerve pain agents, or muscle relaxants when appropriate.
- Physical therapy to improve flexibility, strengthen core and hip muscles, and correct posture and movement patterns.
- Epidural steroid injections or other image‑guided procedures if pain is persistent or severe.
Surgery (such as microdiscectomy or decompression) may be considered when pain lasts longer than several months despite treatment, when there is progressive weakness, or when imaging shows significant nerve compression. Early evaluation and active management lower the risk that sciatica becomes chronic, which can happen in a minority of patients if nerve irritation goes untreated.
What Kind of Doctor Treats Sciatica?
Because sciatica involves both the spine and nerves, several specialists may be involved in your care. Many people start with a primary care physician, who can evaluate symptoms, order basic imaging or physical therapy, and decide if specialist referral is needed.
Depending on your situation, you might see:
- Physical medicine & rehabilitation (PM&R) physicians or pain management specialists for non‑surgical treatment, medications, and injections.
- Neurologists for detailed nerve and muscle testing, especially if weakness or numbness is prominent.
- Orthopaedic spine surgeons or neurosurgeons when surgery may be an option for significant structural compression.
A standard workup includes a history and physical exam, neurologic testing (strength, reflexes, sensation), and, if symptoms are significant or persistent, imaging such as MRI of the lumbar spine. You should seek medical care if symptoms last more than a couple of weeks, keep returning, or interfere with work, walking, or sleep.
Can a Chiropractor Help with Sciatica?

For some people, chiropractic care is a useful part of a comprehensive plan for sciatica. Chiropractors may use spinal manipulation, mobilization, and soft‑tissue techniques to improve joint motion, reduce muscle tension, and help decrease local irritation in selected patients.
Current guidelines suggest that manual therapies, including chiropractic and physical therapy, can play a role in managing low back and radicular pain when combined with exercise and medical oversight. However, chiropractic care is safest and most appropriate.
- A medical professional has ruled out serious causes and red‑flag symptoms.
- There is no rapidly progressing weakness, loss of bowel or bladder control, or other emergency signs.
Good sciatica care is usually multi‑modal—combining exercise, education, manual therapy, medications, injections, and sometimes surgery—tailored to the individual and the exact source of nerve compression. Choosing a chiropractor who communicates with your medical team and refers for imaging or specialist care when needed helps keep treatment safe and coordinated.
When To See a Doctor About Sciatica
You should see a doctor if sciatica symptoms last more than a couple of weeks, keep coming back, or interfere with normal daily activities. Medical care is also important if you notice numbness, tingling, or weakness in your leg or foot, even if the pain itself is tolerable.
Go to an emergency room right away if you develop severe or rapidly worsening leg weakness, loss of bowel or bladder control, or numbness in the groin or saddle area. Prompt diagnosis allows your team to confirm that what you are feeling is truly sciatica and to build a treatment plan aimed at both short‑term relief and long‑term protection of the nerve.



