How to Know If Your TMS Treatment Is Working: Signs, Timeline, and What to Expect
Many patients notice TMS working through small, gradual changes in mood, energy, and daily functioning over the first several weeks, with full benefits often emerging closer to weeks 4–6 of treatment. This blog should normalize that progress looks different for everyone while encouraging patients to complete the full course and stay in close communication with their care team.
Introduction: What TMS Patients Can Expect
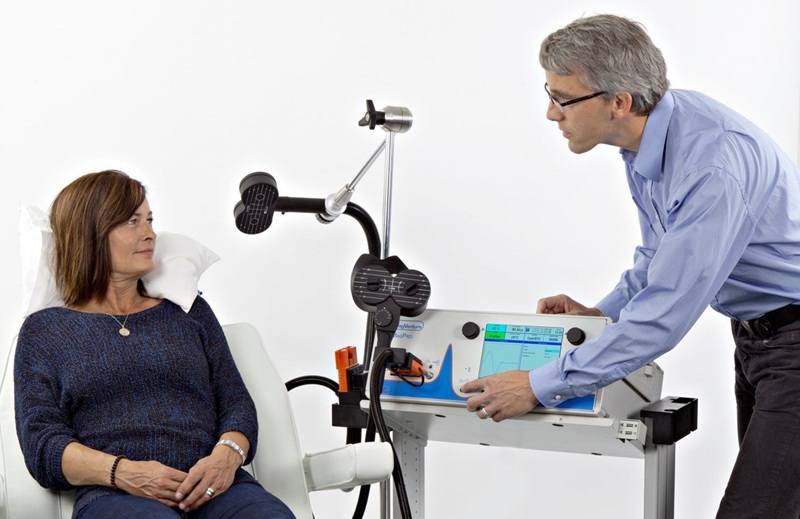
Transcranial Magnetic Stimulation (TMS) is a noninvasive treatment that uses magnetic pulses to stimulate areas of the brain involved in mood regulation, most commonly for treatment‑resistant depression. Many patients start TMS wondering, “How will I know if this is actually working?” and may worry if they don’t feel better right away. This article guides patients through the most common signs of improvement, a realistic week‑by‑week timeline, and practical ways to track progress during their treatment.
Key Signs Your TMS Treatment Is Working
1. Physical changes
Patients often notice physical shifts before they recognize emotional improvements. Common early signs include:
- More consistent, restorative sleep and fewer middle‑of‑the‑night awakenings.
- Gradually increasing energy levels throughout the day and less overwhelming fatigue.
- Feeling less “slowed down” physically, with more capacity to get moving in the morning.
2. Emotional shifts
TMS aims to reduce core symptoms of depression by changing how mood‑related brain circuits function. Emotional signs of progress can include:
- A brighter, more hopeful baseline mood, even if bad days still happen.
- Reduced feelings of worthlessness, guilt, or hopelessness.
- Lower anxiety and irritability, with fewer emotional “crashes” during the day.
3. Cognitive improvements
As mood lifts, thinking often becomes clearer and more organized. Patients may notice:
- Better focus when reading, working, or following conversations.
- Less mental fog or indecision when planning their day.
- An easier time remembering tasks, appointments, or details.
4. Behavioral changes
One of the strongest signs that TMS is helping is a gradual return to everyday activities. These behavioral shifts might look like:
- Renewed motivation to engage in hobbies, exercise, or self‑care routines.
- More consistent follow‑through on basic tasks like showering, cooking, or cleaning.
- Increased social interaction, such as answering messages, making plans, or leaving the house more often.
5. Feedback from people around you
Sometimes, loved ones notice improvements before the patient does. Family or friends might comment that you:
- Seem more present, talkative, or lighthearted.
- Are less withdrawn or less quick to anger.
- Laugh more often or show more facial expression than before.
TMS Timeline: Weeks 1–6 and Beyond

Every brain is different, but clinical studies and patient reports reveal some common patterns in the TMS timeline. It can help to think of progress in stages rather than expecting a sudden “switch.”
Weeks 1–2: Subtle shifts and adjustment
In the first couple of weeks, improvements—if they appear—are often small and easy to miss. During this period, patients may:
- Notice slightly better sleep or a small bump in daytime energy.
- Experience temporary fatigue or mild headaches as the brain adapts to stimulation.
- Feel discouraged if mood has not yet changed much; this is very common and does not mean treatment is failing.
Weeks 3–4: When many people start to notice change
For a large portion of patients, clearer benefits emerge in weeks 3–4. Common changes include:
- Noticeable reduction in depressive symptoms such as sadness, hopelessness, or emotional numbness.
- More stable mood day to day, with fewer deep lows and quicker recovery after stress.
- Better ability to function at work, school, or home as energy, motivation, and focus improve.
By weeks 4–6, many patients experience their most significant gains. Studies show that:
- A majority of patients report substantial symptom relief by this stage.
- Around 30–40% achieve remission, meaning depressive symptoms are minimal or largely resolved.
- Quality of life often improves, with patients describing feeling “more like themselves” again.
After the acute course: Maintaining gains
A standard TMS course usually includes 5 sessions per week for about 6 weeks, totaling roughly 30–36 treatments. After the acute series, many patients maintain improvement for months, sometimes with occasional maintenance sessions if symptoms start to resurface.
How to Monitor Your Progress During TMS

Keep a daily or weekly journal
Writing down your experiences makes gradual change easier to see over time. Patients might track:
- Mood (for example, rating it from 1–10 each day).
- Sleep quality and duration.
Energy levels, anxiety, and motivation. - Activities completed, such as social outings, workdays, or hobbies.
Even small shifts—like going from “unable to get out of bed” to “got up and showered”—are meaningful markers of progress when viewed across several weeks.
Use simple rating scales with your provider
Your TMS team may use standardized depression scales, such as the PHQ‑9 or other symptom checklists, to objectively measure change. Filling these out regularly helps:
- Capture improvements you might minimize or overlook.
- Guide clinical decisions, such as continuing, adjusting, or extending treatment.
Involve trusted family or friends
If you are comfortable, ask a partner, family member, or close friend to share what they notice over time. They can often spot early signs of improvement, like increased engagement or fewer emotional outbursts, that you may not recognize in yourself yet.
Be patient with the process
TMS is designed to produce gradual and cumulative changes in brain function, not an overnight transformation. It is normal to:
- Have ups and downs during treatment, even as the overall trend moves in a positive direction.
- Feel uncertain whether “it’s working” until you look back over several weeks of small improvements.
Why Finishing the Full Course Matters

Even if you feel better early, completing the full recommended TMS protocol is important for solidifying and maintaining gains. Research shows that symptom improvement and remission rates continue to climb over the full series, especially after the third or fourth week.
Patients are more likely to sustain benefits when they:
- Attend sessions consistently and avoid gaps when possible.
- Stay engaged with their broader treatment plan, including therapy or medications when recommended.
- Follow up with their TMS provider to discuss next steps, such as tapering sessions or scheduling maintenance treatments if needed.
If at any point you feel worse, have concerns about side effects, or feel no change after several weeks, it is essential to talk openly with your care team. They may adjust your protocol, review your overall treatment plan, or discuss additional options tailored to your needs.
FAQs About TMS Treatment
How long does it usually take for TMS to start working?
Most patients notice subtle changes in mood, energy, or sleep within the first 2–4 weeks, while more significant improvement often shows up between weeks 4–6 of treatment.
What are early signs that my TMS treatment is working?
Early signs can include sleeping more regularly, having a bit more energy, feeling slightly less hopeless or anxious, and finding it a little easier to get through daily tasks.
What if I don’t feel any better after a couple of weeks?
It’s very common not to notice big changes in the first few weeks. TMS benefits are usually gradual and cumulative, which is why we encourage you to complete the full course unless your provider recommends otherwise.
Can my symptoms get worse before they get better?
Some people feel more tired, irritable, or discouraged early on, especially if they’re hoping for instant results. This doesn’t necessarily mean TMS isn’t working, but you should always tell your provider about any changes.
How will my provider know if TMS is helping me?
We typically use symptom questionnaires, progress check‑ins, and your own reports about mood, sleep, energy, and daily functioning to track changes over time.
What can I do to track my own progress?
Keeping a brief daily journal (rating your mood, sleep, and energy) and noting what you’re able to do—work, social activities, hobbies—can make gradual improvements easier to see.
Why do my friends or family say I seem better when I don’t feel that way?
Loved ones sometimes notice changes in your tone, facial expressions, and behavior before you’re fully aware of them. Their feedback can be a helpful complement to how you feel inside.
Do I still need medication or therapy if TMS is working?
Many patients continue medications or therapy alongside TMS. Any changes to your medications or other treatments should be made in collaboration with your prescribing clinician or therapist.
What happens after I finish my TMS treatment course?
After the acute series, some patients maintain their improvement without additional sessions, while others may benefit from occasional maintenance treatments, depending on symptoms and provider recommendations.
What should I do if I’m worried TMS isn’t working for me?
Reach out to your TMS team as soon as you have concerns. We can review your symptom timeline, adjust your treatment plan if needed, and discuss next steps tailored to your situation.
Want to learn more?
If you are curious whether TMS is right for you—or you are currently in treatment and unsure how to interpret your progress—our clinic team can review your symptoms, timeline, and goals and help you decide on the next best step.