Cervical Herniated Disc: Non-Surgical Relief

What Is a Cervical Herniated Disc?
A cervical herniated disc occurs when the inner gel-like center of a spinal disc (nucleus pulposus) ruptures through its tough outer ring (annulus fibrosus), often pressing on nearby nerve roots or the spinal cord. Most commonly seen at C5–C6 or C6–C7, this condition may cause neck pain, arm numbness, radiculopathy, or even cervical myelopathy in more severe cases.
Though it can result from sudden trauma, herniation typically develops over time due to disc degeneration and mechanical stress.
Anatomy & Pathophysiology
The cervical spine consists of seven vertebrae (C1–C7) and the discs between them. These discs function as shock absorbers, maintaining flexibility and spacing.
With age:
- Discs lose water content → Reduced height and elasticity
- Annular tears occur → Allowing disc material to herniate
- Herniated material compresses nerve roots or the spinal cord
- Local inflammation and chemical irritation intensify nerve pain
This process often leads to radiculopathy (nerve root symptoms) or, in severe cases, myelopathy (spinal cord dysfunction).
Symptoms of Cervical Disc Herniation
Common Symptoms:
- Neck pain: Can be localized or radiate to the shoulders
- Radicular pain: Shooting pain into the arm, forearm, or hand
- Numbness or tingling: Follows a dermatomal pattern (C5–C8)
- Muscle weakness: In shoulder, arm, or hand (grip or biceps)
- Reduced reflexes: Especially biceps (C5–C6) or triceps (C7)
Red Flags for Myelopathy:
- Gait instability or leg weakness
- Loss of hand coordination
- Bowel or bladder dysfunction
- Electric-shock sensation with neck flexion (Lhermitte’s sign)
How We Diagnose a Cervical Herniated Disc
Clinical Assessment:
- Spurling’s test: Reproduces radicular symptoms with neck compression
- Shoulder abduction relief test: Symptom reduction when hand is rested on head
- Dermatome and reflex mapping for level-specific diagnosis
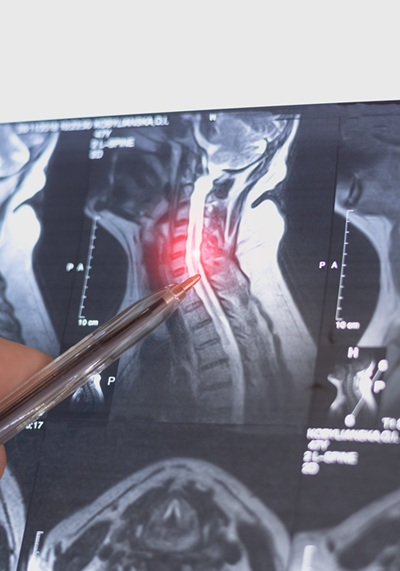
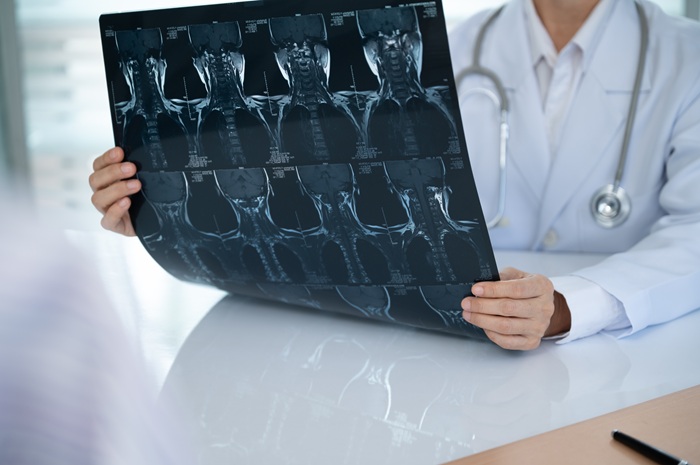
Imaging:
- MRI (gold standard): Reveals disc herniation, nerve impingement, and cord compression
- CT/Myelography: Used when MRI is contraindicated or in post-op evaluations
- X-rays: Identify alignment issues or disc space narrowing
Electrodiagnostics:
- EMG/NCS to confirm nerve root involvement, differentiate from brachial plexus or peripheral nerve disorders

Non-Surgical Treatment Options
We specialize in avoiding surgery through a personalized, multi-modal, evidence-based care model that treats the root cause—not just the pain.
Conservative First-Line Treatments
- NSAIDs for inflammation
- Short taper of oral steroids in acute flare-ups
- Activity modification, not prolonged rest
- Targeted chiropractic or physical therapy focused on cervical stabilization and neural glides
Holistiq’s Cervical Disc Recovery Program
1. Functional & Anti-Inflammatory Nutrition
Customized meal planning with:
- Omega-3 fatty acids, magnesium, turmeric
- Antioxidants to reduce systemic inflammation
- Gut-friendly, hormone-balancing protocols
2. Shockwave Therapy
A non-invasive modality that:
- Stimulates healing with high-energy acoustic waves
- Breaks up scar tissue and chronic muscle tightness
- Supports disc repair and mobility restoration without injections or surgery
3. Peripheral Magnetic Stimulation (PMS)
A non-invasive modality that:
- Enhances deep spinal muscle neuromuscular reactivation
- Reduces nerve irritation,
- Improves cervical spine stabilization
4. Chiropractic & Manual Therapy
- Gentle spinal adjustments and traction
- Cervical decompression techniques
- Myofascial release and active mobilization
5. Image-Guided Injections
- Regenerative biologics (PRP, stem cells) in select cases to promote annular repair
- Cervical epidural steroid injections for acute nerve root inflammation
- Medial branch blocks or radiofrequency ablation if facet joint pain coexists
6. Brain-Body Optimization
- TMS for pain processing
- Mindfulness and CBT
- Neural glides, core stability, gait retraining
- Ergonomic coaching
7. Movement Restoration & Rehab
- Cervical isometrics, nerve glides, and cervical stabilization
- Postural re-training and ergonomic modifications
- Progressive return to activity and prevention of recurrence
When Is Surgery Necessary?
Most patients improve without surgery. However, surgical intervention (e.g., ACDF, disc replacement, or laminoforaminotomy) may be recommended if:
- Severe or worsening motor weakness
- Myelopathy with cord compression
- Persistent pain >12 weeks despite full conservative treatment
- Failed conservative + interventional care
We collaborate with leading neurosurgeons when necessary—and optimize outcomes with pre- and post-surgical regenerative care.
Cervical Disc Herniation FAQ
Q: Can a herniated disc heal on its own?
A: Yes, many reabsorb or scar down naturally with time, especially with the right therapy.
Q: Is surgery always required for cervical radiculopathy?
A: Not at all. Most patients improve with personalized, non-surgical treatment within 6–12 weeks.
Q: Can I work out with a cervical disc issue?
A: Yes, under guidance. Targeted exercise is part of recovery—especially when monitored by Holistiq’s rehab team.
Q: Is neck cracking safe?
A: Self-manipulation isn’t advised. Our spine specialists use precise, safe manual techniques when indicated.
Why Choose Holistiq Spine?
- Functional Diagnostics. Not Just MRI.
- Root Cause + Whole-Person Healing
- Integrated Team Under One Roof
- Cutting-Edge, Non-Surgical Technologies
- Evidence Meets Empathy in Every Plan
Final Thoughts
A cervical herniated disc doesn’t mean you need surgery or lifelong pain meds. At Holistiq Spine & Orthopaedic, we offer innovative, non-invasive, regenerative care that restores function, relieves pressure, and empowers you to live pain-free—naturally.
Schedule your personalized evaluation today and experience spine care the Holistiq way.
Where Does It Hurt? We Can Help.