PRP vs Stem Cell Therapy for Pain & Injuries
Which Treatment Is Right for You?
PRP and stem cell therapy are both regenerative medicine options for pain and injuries, but they are not the same treatment and they are not interchangeable for every case. In general, PRP is simpler and less invasive because it uses concentrated platelets from your own blood, while stem cell therapy is typically more involved because it uses regenerative cells, often harvested from bone marrow or adipose tissue, to support repair in more complex or stubborn conditions.
Understanding PRP vs. Stem Cell Therapy for Pain & Injuries
If you are comparing PRP vs. stem cell therapy, the most important difference is how each treatment works. PRP uses a concentrated portion of your own blood that contains platelets and growth factors to support healing and reduce inflammation, while stem cell therapy uses regenerative cells that may help modulate inflammation and support tissue repair in a broader way.
Both treatments are being studied and used for musculoskeletal conditions such as arthritis, tendon injuries, ligament injuries, cartilage injuries, muscle tears, plantar fasciitis, rotator cuff problems, and other orthopedic pain conditions. A 2024 review found that both PRP and stem cell injections were associated with improved quality of life, quicker return to activities of daily living, and no significant adverse events in the studies reviewed, but it also emphasized that it remains difficult to compare them directly because treatment protocols are not standardized across studies.
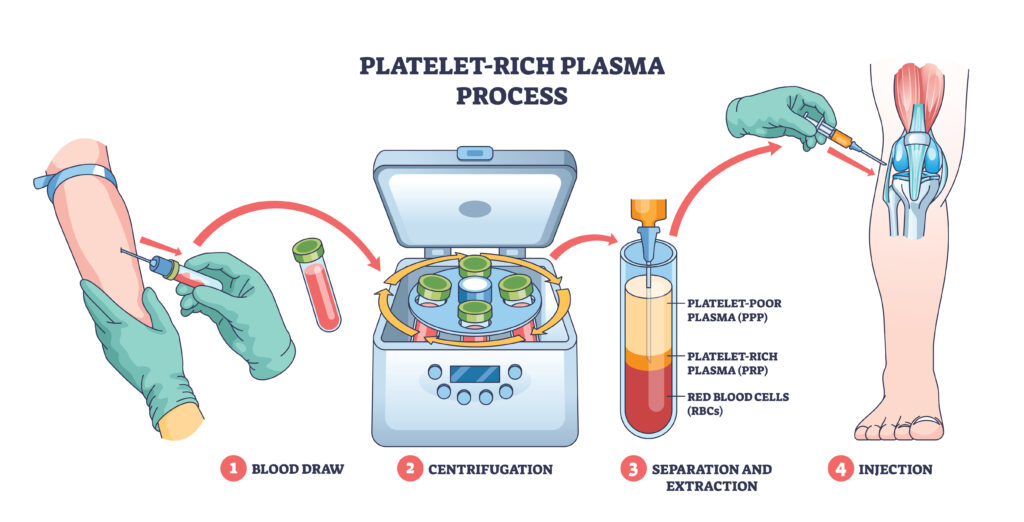
What Is PRP?
PRP, or platelet-rich plasma, is made by drawing a sample of your blood, processing it, and concentrating the platelets before injection into the injured or painful area. Its main effect comes from growth factors that may help reduce inflammation and support the body’s healing response in tendons, ligaments, joints, and other soft tissues.
PRP is often discussed for tendon injuries, ligament sprains, knee osteoarthritis, plantar fasciitis, muscle strains, and some post-surgical orthopedic uses. In the musculoskeletal review, PRP was linked to benefits in conditions such as plantar fasciitis, Achilles tendinopathy, MCL knee injury, chondral knee injuries, muscle tears, and rotator cuff lesions, although some studies found stronger benefits than others.
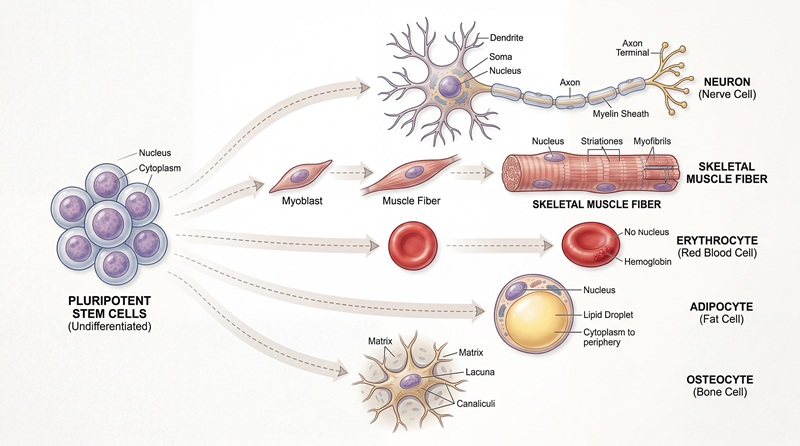
What Is Stem Cell Therapy?
Stem cell therapy for orthopedic pain typically uses adult mesenchymal stem cells, often from bone marrow or adipose tissue, which are harvested, processed, and then injected into the injured area. These cells are being studied because they may help regulate inflammation and support repair processes in cartilage, tendon, ligament, and bone-related injuries.
Stem cell therapy is commonly discussed for osteoarthritis, cartilage defects, chronic joint pain, tendon or ligament injuries, and more difficult degenerative problems. In a meta-analysis of knee osteoarthritis trials, nine randomized controlled trials involving 339 patients found improved pain outcomes in stem cell groups compared with controls, although not every functional measure showed a significant difference at each follow-up point.
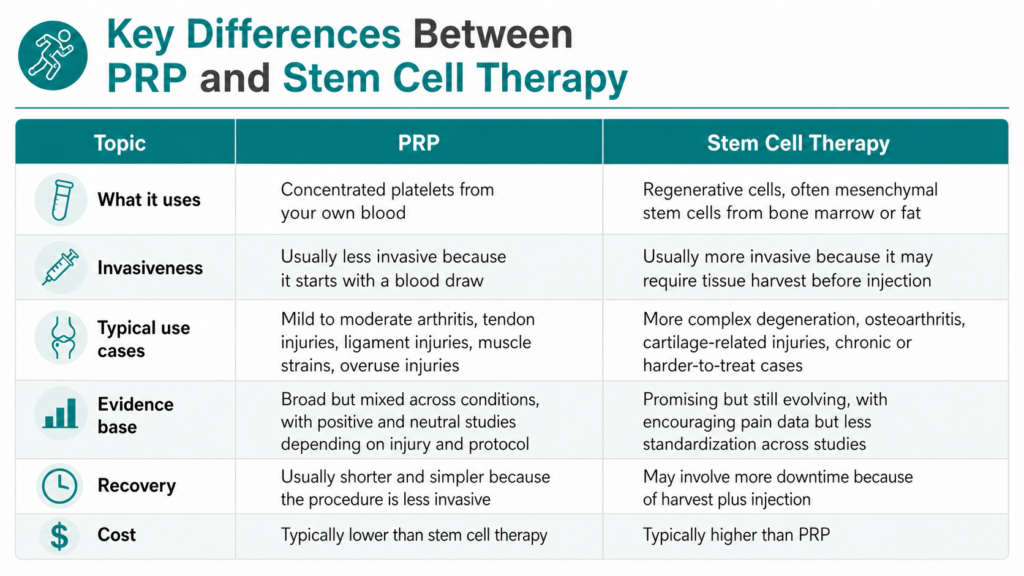
Pros and Cons of PRP Therapy
Pros of PRP
- PRP is minimally invasive and usually begins with a simple blood draw.
- It may help reduce pain and improve function in a range of musculoskeletal injuries and arthritis-related conditions.
- It generally has a favorable safety profile because it uses your own blood product, and the 2024 review described PRP and stem cell approaches as effective and safe in certain musculoskeletal injuries without significant adverse events in the reviewed studies.
- It is usually easier and less costly to perform than stem cell therapy.
- Recovery time is typically shorter with less downtime.
Cons of PRP
- PRP is not equally effective for every injury, and some studies in Achilles tendon problems and other conditions showed little or no significant difference from control treatments
- Results may be more modest in advanced degeneration because PRP mainly amplifies the body’s existing healing response rather than adding harvested regenerative cells.
- It may require repeat injections depending on the condition and response.
- Research protocols vary widely, which makes outcomes less predictable across clinics and conditions.
Pros and Cons of Stem Cell Therapy
Pros of Stem Cell Therapy
- Stem cell therapy may offer broader regenerative potential in harder-to-treat or more degenerative conditions because it uses living regenerative cells rather than platelets alone.
- In knee osteoarthritis research, stem cell therapy showed better pain improvement than control treatments at 3, 6, and 12 months in a meta-analysis of nine randomized controlled trials.
- It may be considered for cartilage-related injuries, chronic joint pain, and more advanced wear-and-tear problems where a provider wants a more aggressive regenerative approach.
- The knee osteoarthritis meta-analysis found no significant increase in adverse events versus controls in the included trials.
Cons of Stem Cell Therapy
- Stem cell therapy is usually more invasive because it may require harvesting cells from bone marrow or adipose tissue before injection.
- It is usually more expensive than PRP.
- The evidence remains mixed, and not every outcome measure in the knee osteoarthritis meta-analysis showed significant functional superiority over controls at every time point.
- Research and protocols are not standardized, which makes comparisons across studies and clinics difficult.
- Recovery may involve more downtime than PRP due to the tissue harvest procedure.
Which Is Better for Pain and Injuries?
Neither PRP nor stem cell therapy is automatically “better” for every patient, because the right option depends on the condition being treated, how severe the tissue damage is, the goals of treatment, and how invasive a procedure the patient wants to consider. The current literature supports both treatments as potentially useful for certain musculoskeletal problems, but it also shows mixed results and a lack of standardized protocols, so the best choice should be based on diagnosis, imaging, severity, prior treatment response, and a personalized evaluation rather than hype.
A practical way to frame the difference is this: PRP is often easier to start with when the issue is inflammation, tendon dysfunction, or mild-to-moderate degeneration, while stem cell therapy may be considered when the case is more complex, chronic, or structurally degenerative and a broader regenerative strategy is being considered.
Frequently Asked Questions
What is the main difference between PRP and stem cell therapy?
PRP uses concentrated platelets and growth factors from your blood, while stem cell therapy uses regenerative cells, often taken from bone marrow or fat, to support repair and healing.
Is PRP safer than stem cell therapy?
Both treatments appear to have favorable safety profiles in the reviewed musculoskeletal literature, and the 2024 review reported no significant adverse events in the studies it summarized. In knee osteoarthritis trials, stem cell therapy also did not show a significant increase in adverse events compared with control groups in the meta-analysis.
Is PRP cheaper than stem cell therapy?
Yes, PRP is typically less expensive than stem cell therapy according to comparative pricing summaries in current clinical comparison sources.
Does stem cell therapy work better than PRP?
Not always. Some comparative sources and trial summaries suggest stem cell therapy may be useful in more advanced or difficult cases, but direct comparisons do not consistently show superiority, and one comparison summary noted no superiority of a single bone marrow concentrate injection over a single PRP injection for moderate knee osteoarthritis.
Which treatment is better for arthritis?
Both PRP and stem cell therapy are used for arthritis, especially knee osteoarthritis, but the better choice depends on severity, goals, prior treatments, and how invasive an option the patient is willing to pursue. PRP is often considered first because it is simpler, while stem cell therapy may be considered in selected more challenging cases.
Which treatment is better for sports injuries?
PRP is commonly used in sports medicine for tendon, ligament, and muscle injuries and has shown faster return-to-play or symptom improvement in some studies, though not in all conditions. Stem cell therapy may be considered in more complex or persistent injuries, but the evidence base is still evolving.
How long do results last?
PRP typically has a shorter recovery time because it is less invasive, starting with just a blood draw. Stem cell therapy may require more recovery time due to the tissue harvest procedure.
Can PRP and stem cell therapy be combined?
Some providers combine PRP with stem cell therapy for certain complex cases, though research on combined approaches is still limited. This decision should be based on individual evaluation and clinical judgment.
Which has a faster recovery time?
PRP typically has a shorter recovery time because it is less invasive, starting with just a blood draw. Stem cell therapy may require more recovery time due to the tissue harvest procedure.
Take the First Step Toward Pain-Free Movement
Schedule your consultation today to explore which regenerative medicine option—PRP, stem cell therapy, or a combination approach—may help you find relief and return to the activities you love. Our team will review your specific case and create a personalized treatment plan designed around your needs and goals.
Where Does It Hurt? We Can Help.




Regenerative Medicine
